We’ve talked a lot about T cells and MHC proteins and how they recognize gluten. But B cells also play a key role in celiac disease.
Like T cells, B cells have receptors (B cell receptor or BCR) on their surfaces that recognize specific pathogens. Unlike T cells, they do not need antigen presenting cells to display a pathogen peptide for them—they are able to recognize pathogens on their own. Each B cell has a unique type of B cell receptor that is capable of recognizing only a few antigens.
When a B cell bumps into a pathogen that it recognizes, it brings the whole pathogen into the cell and digests it into peptides. As discussed above, B cells are antigen presenting cells and display pathogen peptides on their surface in complex with an MHC class II molecule. They do this because they need the help of Th2 helper T cells to become activated. Th2 helper T cells that have already recognized the same pathogen (by interacting with other antigen presenting cells) are able to recognize the antigen displayed by the B cell. When this happens, Th2 cells produce cytokines that cause the B cell to mature into a plasma cell.
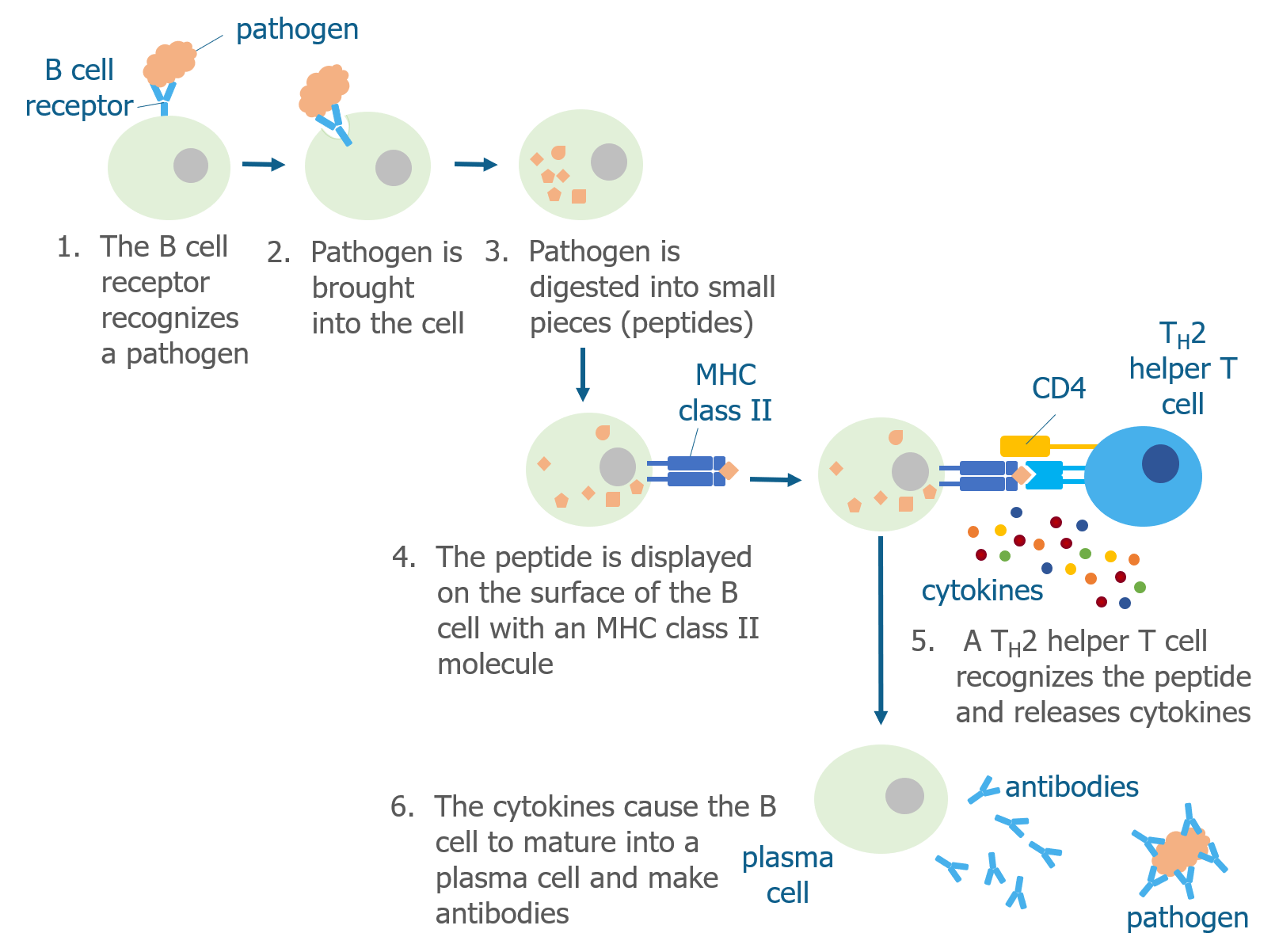
The main role of plasma cells is to produce proteins called antibodies (also known as immunoglobulins), which are Y-shaped proteins that recognize the same pathogen that the B cell originally recognized. Plasma cells release these specific antibodies into the surrounding tissue where they find and stick to the pathogen.
By doing this, antibodies stop the pathogen from spreading and mark it for destruction by other immune cells. This type of immune response is often called the antibody-mediated immune response.
There are five main classes of antibodies—IgA, IgD, IgE, IgG, and IgM—each of which have different roles. Two of these classes, IgA and IgG, can be found at high levels in blood samples.
How Are B Cells Involved in Celiac Disease?
In the 1980s, researchers discovered that patients with celiac disease had high levels of antibodies that recognized gliadin (a protein in gluten) in their small intestine.1 Patients with celiac disease were also found to have auto-reactive antibodies—that is, antibodies that recognize normal “self” proteins.
Researchers developed a blood test that was able to detect IgA antibodies that recognized a type of tissue called endomysium.2 In 1997, Dr. Detlef Schuppan and his team discovered that IgA antibodies in the blood of patients with celiac disease recognized a specific protein in the endomysium—a protein called tissue transglutaminase (tTG).3 The antibodies to gliadin, endomysium, and tTG disappear when patients adopt a gluten-free diet, which suggests that these antibodies are made as part of an immune response to gluten.
We know that T cells can recognize deamidated gliadin peptides and begin an immune response, so it makes sense that B cells might produce antibodies to gliadin if they mistakenly recognize it as a pathogen. But why would B cells produce antibodies to tTG, a normal protein in the body?
As we discussed above, tTG is the enzyme that is responsible for converting the glutamine amino acids into glutamate amino acids to produce deamidated gliadin peptides, which have increased immunogenicity. In addition to changing glutamines to glutamates, tTG can also cross-link the gluten peptide to itself.
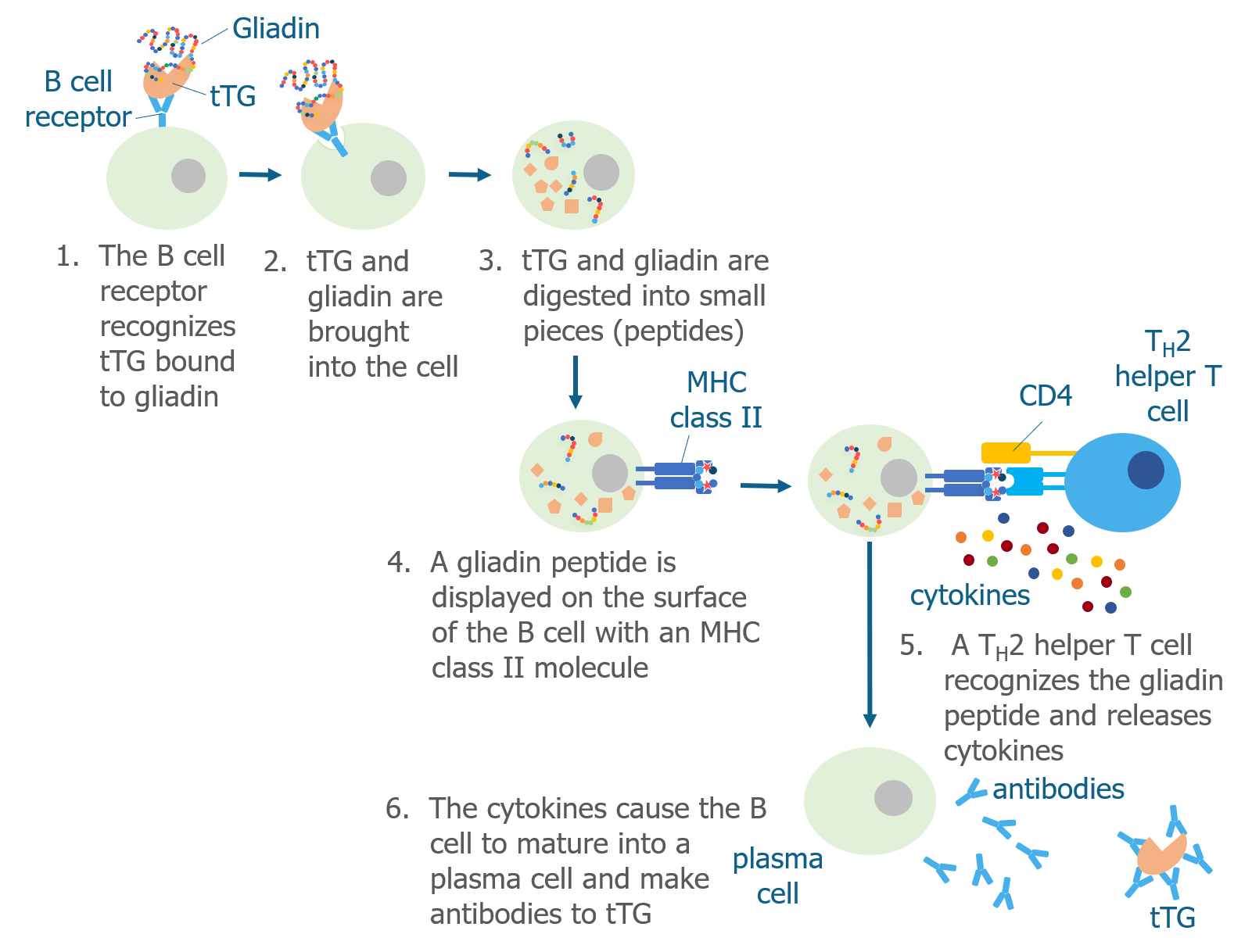
Researchers are still trying to understand exactly how gluten causes B cells to make antibodies that recognize tTG, but they think that B cells ingest tTG that is cross-linked to a gliadin peptide. Then, Th2 helper T cells that recognize gliadin help B cells produce antibodies to tTG.
REFERENCES
- Mesin L, Sollid LM, Di Niro R. The intestinal B-cell response in celiac disease. Front Immunol. 2012;3:313.
- Chorzelski TP, Sulej J, Tchorzewska H, Jablonska S, Beutner EH, Kumar V. IgA class endomysium antibodies in dermatitis herpetiformis and coeliac disease. Ann N Y Acad Sci. 1983;420:325-334.
- Dieterich W, Ehnis T, Bauer M, et al. Identification of tissue transglutaminase as the autoantigen of celiac disease. Nat Med. 1997;3(7):797-801.
GLOSSARY
Antibodies – Y-shaped proteins that recognize foreign pathogens. Made by B cells. Also called immunoglobulins.
Antibody-mediated immune response – An immune response that involves the production of antibodies. Also known as the humoral immune response.
Antigen – A protein that is recognized by an immune cell receptor and triggers an immune response.
Antigen presenting cell – A specialized immune cell that presents peptides to CD4+ or CD8+ T cells. Peptides are presented by MHC I or MHC II proteins.
B cell – A type of adaptive immune cell. Also called B lymphocyte.
Cytokines – Small proteins that are made and released by immune cells. Allows cells to send signals and provide instructions to other cells.
Endomysium – A type of connective tissue.
Enzyme – A protein that can change one type of molecule to another.
Gliadin – One of the wheat proteins that forms gluten. Responsible for triggering an immune response in patients with celiac disease.
Gluten – A type of protein found in cereal grains. Wheat gluten is made of two proteins called gliadin and glutenin.
Helper T cell – Adaptive CD4+ immune cell that produces cytokines when activated.
Immunogenicity – The ability of an antigen to induce an immune response.
MHC class I protein – Major histocompatibility complex class I protein. Found on the surface of normal cells. Presents peptides to CD8+ T cells.
MHC class II protein – Major histocompatibility complex class II protein. Found on the surface of antigen presenting cells. Presents peptides to CD4+ T cells.
Pathogens – Bacteria and viruses that can cause disease.
Peptide – A small protein fragment consisting of a chain of amino acids.
Plasma cell – Mature B cell that can produce antibodies.
T cell – A type of adaptive immune cell. Also called T lymphocyte.
Tissue transglutaminase (tTG) – An enzyme that deamidates gliadin peptides causing them to be more immunogenic. Also the target of auto-antibodies in patients with celiac disease.
Share this Post
One Comment on “B Cells”
Your way of presentation and explanation of concepts is pleasantly unique. Those little illustrations help to understand the concepts with clarity.