We have talked about the different types of immune cells, how they mistakenly recognize gluten, and how they make antibodies to tissue transglutaminase (tTG). But these things don’t happen in isolation—several things must happen at the same time for damage to the small intestine to occur.
First, gluten must be eaten and digested in the stomach and small intestine. Since gliadin is hard to digest, small peptides remain in the intestine. These peptides then cross the epithelium (cell layer) into the mucosa. Researchers are still trying to understand how this happens. Certain proteins, such as zonulin, may make the cell layer more permeable, so peptides can pass through to the underlying mucosal layer.1
Once the gliadin peptides get to the mucosal layer, they become modified by tissue transglutaminase (tTG) to fit better within the grooves of the MHC class II proteins on antigen presenting cells. Only antigen presenting cells with HLA-DQ2 or HLA-DQ8 haplotypes are able to present deamidated gliadin peptides and activate CD4+ T cells.
Once the CD4+ T cells are activated, they produce Th1 helper T cells, which make cytokines that recruit and activate other innate immune cells and CD8+ intraepithelial lymphocytes (IELs). Th17 cells, which play a role in many autoimmune diseases, are also involved in celiac disease. Activated Th2 cells may help to activate B cells that recognize tTG, resulting in the production of antibodies against tTG.
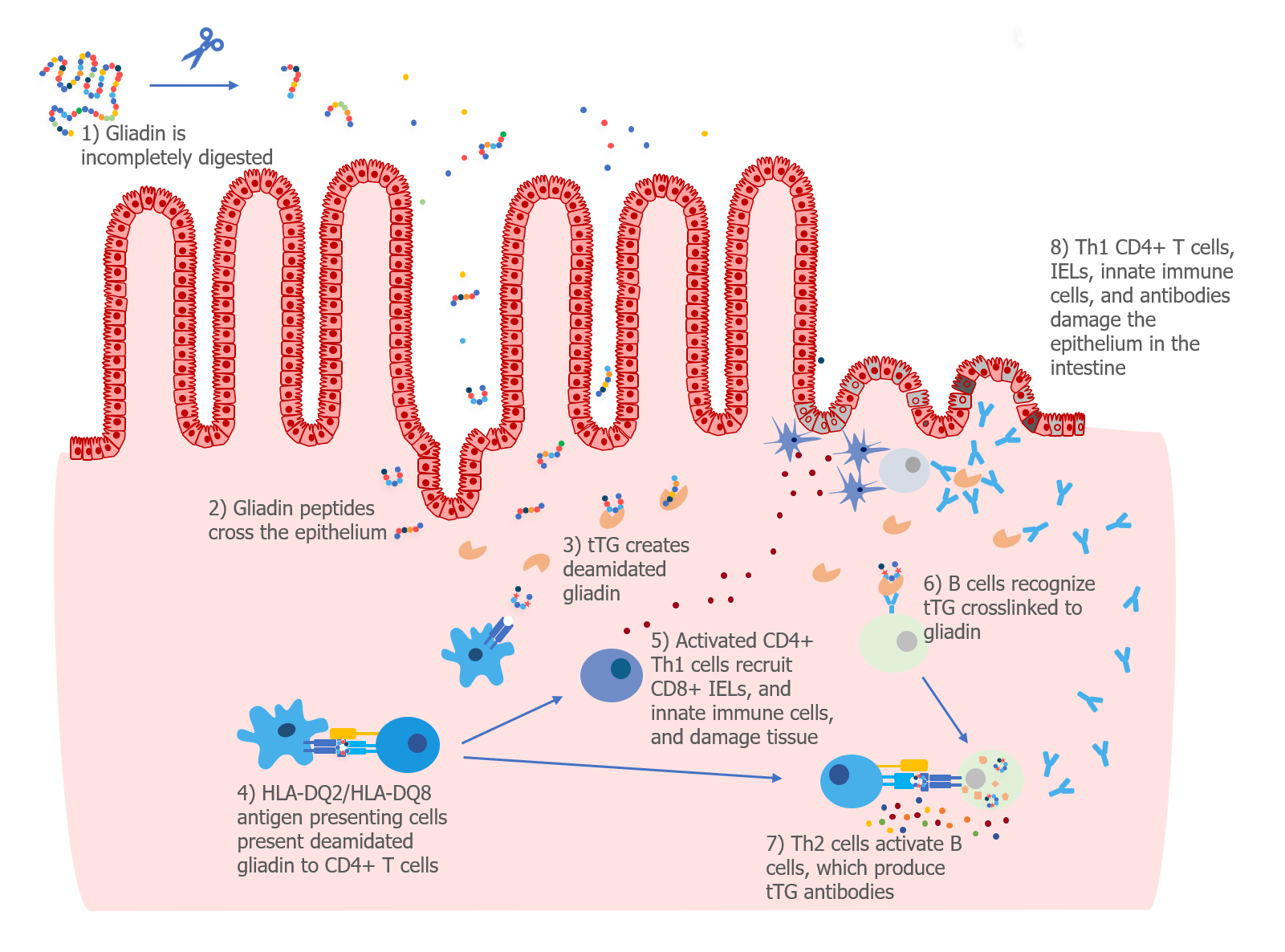
Together, the Th1 CD4+ T cells, IELs, innate immune cells, and antibodies cause inflammation and damage to the cells of the intestine.
Gluten is the trigger for this entire process—if it is removed from the diet, there is no immune response and the intestine is able to heal.
REFERENCES
- Sturgeon C, Fasano A. Zonulin, a regulator of epithelial and endothelial barrier functions, and its involvement in chronic inflammatory diseases. Tissue Barriers. 2016;4(4):e1251384.
GLOSSARY
Antibodies – Y-shaped proteins that recognize foreign pathogens. Made by B cells. Also called immunoglobulins.
Antigen presenting cell – A specialized immune cell that presents peptides to CD4+ or CD8+ T cells. Peptides are presented by MHC I or MHC II proteins.
B cell – A type of adaptive immune cell. Also called B lymphocyte.
CD4 – A co-receptor on the surface of helper T cells.
CD8 – A co-receptor on the surface of cytotoxic T cells.
Cytokines – Small proteins that are made and released by immune cells. Allows cells to send signals and provide instructions to other cells.
Gliadin – One of the wheat proteins that forms gluten. Responsible for triggering an immune response in patients with celiac disease.
Gluten – A type of protein found in cereal grains. Wheat gluten is made of two proteins called gliadin and glutenin.
Haplotype – Variations in HLA genes that produce different MHC class II proteins.
Helper T cell – Adaptive CD4+ immune cell that produces cytokines when activated.
Immune cells – Specialized white blood cells (also called leukocytes) that fight infection.
Intraepithelial lymphocytes – Cytotoxic CD8+ T cells that reside in the intestine. Contribute to tissue damage in celiac disease.
MHC class I protein – Major histocompatibility complex class I protein. Found on the surface of normal cells. Presents peptides to CD8+ T cells.
MHC class II protein – Major histocompatibility complex class II protein. Found on the surface of antigen presenting cells. Presents peptides to CD4+ T cells.
Pathogens – Bacteria and viruses that can cause disease.
T cell – A type of adaptive immune cell. Also called T lymphocyte.
Tissue transglutaminase (tTG) – An enzyme that deamidates gliadin peptides causing them to be more immunogenic. Also the target of auto-antibodies in patients with celiac disease.
Share this Post
